(Download)
The Public Health Emergency Playbook is a guide designed for Governors and their staff, offering a comprehensive resource to effectively prepare for, manage, and recover from health crises across a range of health emergencies, including natural disasters, infectious disease outbreaks, industrial accidents, and human-caused disasters. It outlines steps Governors can take to enhance preparedness efforts as well as provides a checklist of potential actions for Governors to consider when responding to and recovering from a public health emergency. This Playbook also addresses the intricate dynamics of public health emergencies, emphasizing a comprehensive and holistic “one health” approach. By recognizing the diversity of these crises, Governors can employ targeted preparedness and response efforts to safeguard their States, Commonwealths, and Territories, herein referred to as states.
Below are several key steps Governors and their teams can take to prepare for, respond to, and recover from a public health emergency:
Preparing for a Public Health Emergency
- Engage in Critical Incident Response Planning: Work with public health and emergency management officials to review the current state of readiness, exercise, and adjust existing emergency operations planning to align with the Governor’s priorities and maximize public safety.
- Advance Legal Preparedness: Identify gubernatorial and state health department emergency authorities and a process for working with the chief legal counsel to vet and issue any executive orders that may be needed during a public health emergency.
- Sustain Disaster Funding: Regularly evaluate state response funding levels and mechanisms, as well as available federal dollars, to address public health emergencies, particularly given the increased frequency, scale and concurrence of disasters.
- Support Public Health and Healthcare Workforce Efforts: Evaluate current and projected workforce needs and explore recruitment, development, and resiliency strategies across the state, including in underserved communities.
- Bolster Public Health Infrastructure: Invest in public health infrastructure to include data systems, access, and workforce, to ensure the Governor has the information needed to make critical decisions in future emergencies and that communities have access to resources and care.
- Champion Public Health Communications: Regularly and intentionally engage with the public through consistent platforms to identify where trusted health information can be transmitted both on a day-to-day basis and during an emergency.
Responding to a Public Health Emergency
- Call on Key Leaders: Bring together public health, emergency management and other officials to assess the situation, identify resource needs, understand potential impacts, and if needed, activate an incident response plan.
- Take Executive Action: Exercise gubernatorial emergency powers to take actions to support the response, as needed, such as surging resources, enacting anti-price gouging restrictions, and temporarily waiving rules and regulations that may hinder responders.
- Obtain and Allocate Resources: Leverage state and local resources or stockpiles to support impacted areas and coordinate with federal, inter-state and private partners to fill resource gaps—prioritizing the allocation of resources to those with the greatest need.
- Marshal Financial Resources: Monitor budgetary needs for the response and regular government services, leverage federal funding or additional state appropriations, as well as other funding sources, including private, philanthropic, or other non-governmental resources. Maintain transparency and thorough record keeping throughout the emergency.
- Communicate Regularly and Intentionally: Maximize communication channels with the public, be mindful of the best mediums to reach underserved communities, and centralize critical information into easily accessible and digestible hubs to minimize the potential impact of mis- or dis-information.
Post-Response & Recovery from a Public Health Emergency
- Address Long-term Needs: Work with public health officials to monitor community health impacts and allocate additional resources to support recovery and any individuals facing long-term health effects.
- Support Community & Responder Mental Health and Well-Being: Evaluate mental health needs for those impacted, including responders, and leverage federal, state, local, or private resources to ensure access to care.
- Continue Regular Communications Through Recovery: Regularly engage with the public throughout the recovery process, provide information on available resources, actions the public can take, and anticipated timelines, being responsive to community input and needs.
- Ensure Lessons Learned Inform Future Response Efforts: Task agencies with conducting an after-action review of the effectiveness of the response, identify areas for improvement, and adjust existing operating procedures to institutionalize these best practices.
The Playbook was developed through significant research and extensive interviews with federal, state, and local entities to capture best practices. The Playbook was also informed by insights from state and territorial leaders at a 2023 workshop focused on preparing for future public health emergencies that was jointly hosted by NGA and the Association for State and Territorial Health Officials. Collectively, the perspectives of more than 30 states and territories, as well as key federal agencies, contributed to the development of the Playbook. This Playbook was prepared by the NGA Center for Best Practices in consultation with Avoq. This work was supported by the Centers for Disease Control and Prevention (CDC) of the U.S. Department of Health and Human Services (HHS). The contents of this publication are the sole responsibility of the authors and do not necessarily represent the official views of, nor an endorsement, by CDC/HHS, or the U.S. Government.
UNDERSTANDING PUBLIC HEALTH EMERGENCIES
Public health emergencies are dynamic and multifaceted, ranging from localized incidents to global crises, underscoring the need for adaptable response strategies. This section delves into the scale of public health threats, exploring how they impact communities and regions. Additionally, it underscores the importance of adopting a “one health” approach, recognizing the interconnectedness of human, animal, and environmental health. Understanding these intricate connections is vital for effective response and mitigation efforts in the face of public health challenges.
Types Of Health Threats
Health crises can strike in many ways, and each one requires a distinct set of preparedness, response, and recovery strategies. Governors’ offices work with federal, state, local, tribal and territorial responders to develop comprehensive and effective strategies for addressing potential threats and resourcing the response accordingly. Public health threats have both short-term and long-term consequences that are important to factor in. For instance, a wildfire may have immediate impacts for those injured by fire or destruction, an intermediate physical health impact of respiratory illnesses from smoke inhalation, and long-term physical or mental health impacts. Categories of health threats may include:
- Natural Disasters: These are events caused by natural forces such as hurricanes/typhoons, floods, earthquakes, or wildfires. They may disrupt critical infrastructure, including healthcare services, and increase injuries and illness.
- Infectious Disease Events: These are crises surrounding the spread of an infectious pathogen, leading to an abnormal number of infections in a population over a short period of time. These outbreaks can remain localized or, in severe cases, spread to become epidemics or pandemics.
- Major Industrial Accident: Major industrial accidents typically result from within industrial facilities, leading to the release of hazardous substances into the environment, such as chemical spills. These incidents can have a wide range of health consequences, spanning
from immediate physical injuries to enduring conditions resulting from exposure to
harmful chemicals. - Human-Caused Disasters: These are events that result in significant harm, including loss of life, injury, or other negative health impacts. Human-caused disasters can be intentional, such as acts of terrorism or bioterrorism, or unintentional, like some mass transportation accidents or infrastructure failures.
- Other Public Health Threats: Some crises evolve over an extended period without a clear, acute onset, such as the opioid crisis. These health crises can cause significant harm, including increased rates of morbidity and death, over long timeframes.
State And Federal Declarations
The types of declarations below provide a framework for understanding the levels of response and the resources available at various stages and types of declarations. In general, emergencies and disasters are coordinated at the level of government closest to the impacted area (e.g., local/county government) until it exceeds their capacity, at which time a leader may request it to be elevated to a higher level of government. If a state or territory exceeds its capacity to respond, it may request federal disaster assistance in line with the mechanisms outlined below. Having a clear understanding of these designations and the resources and authorities they provide can help to ensure an effective and coordinated response to public health emergencies.
Figure 1.
| Type of Emergency Declaration | Description | Impact on States and Territories | Governor’s Role in the Declaration Process |
|---|---|---|---|
| State of Emergency or Disaster | Temporarily enhances the state government's authority and allows it to take specific actions to address an emergency situation. | Allows states to allocate additional resources, mobilize personnel, activate emergency response plans, and regulate certain activities. It can also facilitate the release of emergency funds. | The Governor assesses the situation, determines the need for enhanced powers and resources, and issues an official declaration. |
| State Public Health Emergency | Specific type of state of emergency available in many states, declared in response to a public health crisis such as an infectious disease outbreak or a bioterrorism threat. | May allow state health agencies to take specific actions to address the health crisis, such as quarantining individuals, mobilizing medical resources, providing guidance to healthcare providers, and implementing disease surveillance measures. | Typically declared by the state's Governor or a relevant health authority. The definition of a public health emergency and procedure for issuing a declaration may differ from a state of emergency or disaster. |
| National Emergency | Typically issued in response to a situation that poses a significant threat to the nation as a whole, such as natural disasters, acts of terrorism, or other major crises. Use of this for public health emergencies has previously been limited to national pandemics (e.g. COVID-19 and H1N1). | The declaration of a national emergency grants the President additional powers and resources to address the emergency effectively. The U.S. Federal Emergency Management Agency (FEMA) plays a key role in coordinating and supporting the response efforts during a national emergency. | A national emergency is a declaration that can only be made by the President of the United States under the authority of the National Emergencies Act. |
| Stafford Act Emergency Declaration | Any occasion or instance for which, in the determination of the President, federal assistance is needed to supplement state and local efforts and capabilities to save lives and protect property, public health and safety, or to lessen or avert the threat of a disaster in any part of the United States. | Provides immediate federal resources and support, such as equipment, personnel, and financial assistance, to respond to an ongoing or imminent emergency, and is limited to immediate and short-term assistance that is essential to save lives and protect public health, safety, and property. Public Assistance (PA) and Individual Assistance (IA) may be authorized in limited capacities. | Governor must submit a request to the President through the appropriate FEMA Regional Administrator within 5 days after the need for assistance becomes apparent, but not longer than 30 days after the occurrence of the incident, unless an extension request is granted. If the total amount of federal assistance provided exceeds $5 million, FEMA must notify Congress. |
| Stafford Act Emergency Declaration with Federal Primary Responsibility | Occurs when an emergency exists for which the primary responsibility rests with the Federal government. | Similar to a Governor-requested Emergency Declaration, makes certain programs within Public Assistance (PA) and Individual Assistance (IA) available to states/territories. | The President may declare without a request from a Governor. This declaration does not prevent the Governor or Tribal Chief Executive from subsequently requesting a major disaster declaration for other unmet needs caused by the event. |
| Stafford Act Major Disaster Declaration | Any natural catastrophe (including hurricanes, floods, wildfires, or severe storms) or, regardless of cause, any fire, flood, or explosion in any part of the United States which, in the determination of the President, causes damage of sufficient severity and magnitude to warrant major disaster assistance under the Stafford Act. | Federal assistance becomes available to support the affected state/territory. The assistance depends on the nature of the declaration but may include funding for response operations, public health services, infrastructure repairs, and mitigation, as well as individual assistance programs for affected individuals and communities. FEMA assistance approved under a major disaster may include Individual Assistance (IA), Public Assistance (PA), and the Hazard Mitigation Grant Program (HMGP). | Governor must submit a request to the President through the appropriate FEMA Regional Administrator within 30 days of the occurrence of the incident or within 30 days of the end of the incident period, whichever is later, unless an extension request is granted. The request includes an estimate of the amount and severity of damage to the public and private sector, along with additional information. |
| Federal Public Health Emergency | The Secretary of Health and Human Services of the United States (HHS Secretary) may declare a Public Health Emergency (PHE) if they determine that 1) a disease or disorder presents a PHE, or 2) a PHE, including significant outbreaks of infectious diseases or bioterrorist attacks, otherwise exists. A PHE is typically declared in response to a health crisis that poses a significant threat to public health. | This declaration allows HHS to mobilize resources, implement emergency measures, and coordinate a national response to the crisis. The HHS Secretary can also waive certain regulatory requirements after the issuance of an HHS Public Health Emergency and a Presidential disaster or emergency declaration under the Stafford Act or National Emergencies Act. | The HHS Secretary can declare a Public Health Emergency independent of or at the same time FEMA declares an incident as an emergency under the Stafford Act. A Governor is not required to formally request the HHS Secretary to issue a declaration, but they can communicate the need for a PHE to the HHS Secretary through the Assistant Secretary for Preparedness and Response. If needed, they can also work with their HHS Regional Emergency Coordinator, who can help facilitate a request. |
For emergencies that can be identified before they occur, such as a hurricane, states and territories may choose to issue an emergency declaration and request federal, or interstate mutual aid, assistance in advance. This can provide the state with additional readiness and mitigation resources as well as provide for a more rapid response to the incident.
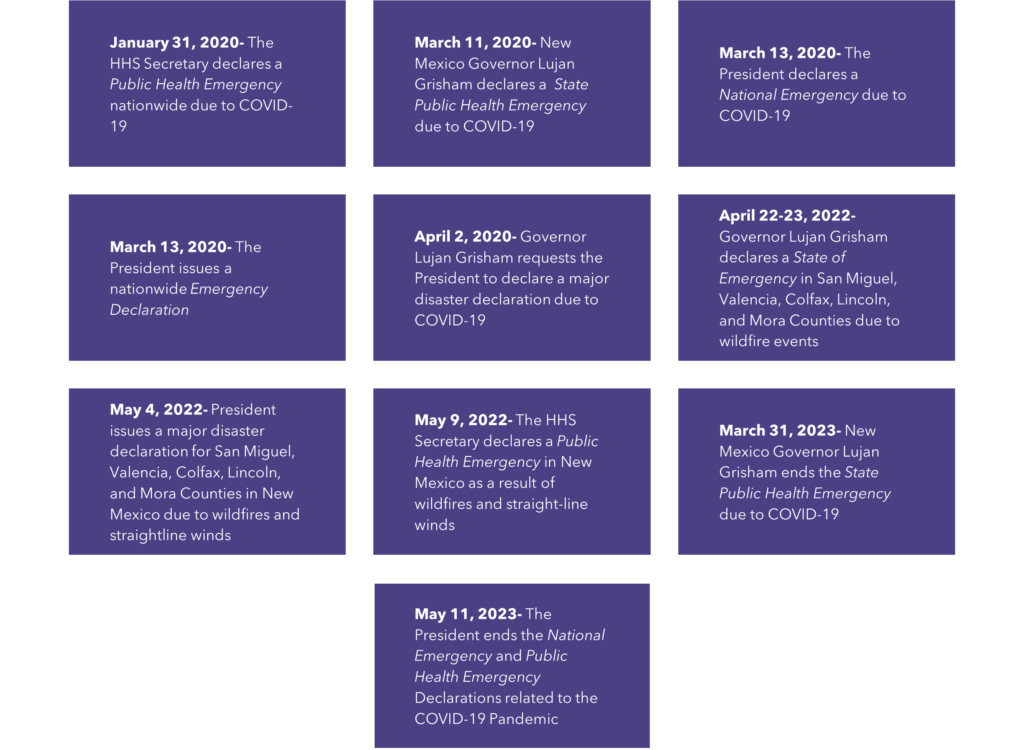
Some incidents may involve multiple types of emergency declarations depending on the type of emergency and the resources needed for response. Additionally, as the pace and severity of emergencies increase, states and territories may face concurrent emergencies. State and federal actions may be exercised simultaneously for the same incident, and there may also be multiple incidents within that same window. Governors’ offices lead these efforts and support state health officials, emergency managers, and other responders in addressing emergencies by providing clear priorities, rallying resources, amplifying public communications, and supporting coordination of community-wide efforts across state agencies. Figure 2 demonstrates an example of concurrent emergencies and the use of multiple, overlapping declarations in New Mexico.
Figure 2.
The preparedness section of this document provides information on ways Governors’ offices can support efforts to strengthen public health emergency response efforts in advance of an incident. The response section is intended to provide actionable steps that can be taken during an emergency.
PREPARING FOR A CRISIS
Governors play a vital role in responding to public health emergencies, both in leading and coordinating preparedness and response efforts. In some instances, Governors may need to initiate some emergency actions or orders to provide the necessary resources and authorities to responders to address the incident. Proactive planning helps to:

Ensure a rapid,
effective response

Reduce impacts to
the community

Aid in a
faster recovery
This section highlights several key considerations and recommendations for proactive planning efforts, including making use of “steady state” periods to discuss and integrate critical response plans, ensure processes are equitable and infrastructure is scalable, as well as to prepare for the legal and administrative aspects of responding to a public health emergency.
Critical Incident Response Planning
Emergency preparedness begins with appointing key leadership who can support the Governor’s vision and effectively manage operations both during day-to-day activities and during an incident. Governors regularly work with key staff, including state health officials, directors of public health emergency preparedness, and emergency managers. These officials work together regularly to develop plans for incident response and recovery.
State legislators may also have a role in emerging response, including allocating emergency funding, the declaration renewal process, or notice requirements. Governors and state officials may also brief them on the state’s overall response plan and relevant processes prior to a disaster.
Governors may also identify staff and develop processes within their office to work with state agencies and coordinate emergency response. Governors’ Homeland Security Advisors, agricultural officials, and public safety officials may also be key resources in this effort. It is vital to ensure that state plans and Governors’ processes are in alignment. It is also important to make updates when threats or response capabilities change, and to incorporate new lessons learned and best practices. This section highlights several key factors and recommendations for successful proactive planning.
Public Health Emergency Response Structure
Public health and emergency management organizations generally use standardized structures for coordinating response efforts across levels of government. Governor’s office involvement in emergency response may vary depending on the scale, pace, and impact of the incident. Providing agencies with information on the Governor’s expectations during a crisis can aid them in more effective preparation and coordination during a response. Governors may choose to lead through a senior policy group, identify a primary point of contact to serve as a conduit for the Governor, directly communicate with the Incident Commander, or use another model.
To ensure alignment between state plans and Governors’ office expectations and processes, it is important to work with public health and emergency management officials on response coordination efforts, including:
- The notification process for critical incidents and emergencies, which may vary depending on urgency and severity (e.g., fatal or time-sensitive incidents may necessitate immediate notification to the Governor or Chief of Staff);
- Governor’s office crisis response posture and how it will work with the response agencies;
- Governor’s office expectations and priorities for emergency response; and,
- The policy decision-making process during an emergency, including the level of involvement of the Governor’s office, coordination with the senior policy group (if applicable), how policy issues will be elevated, and expected timeline for decisions.
Key State Health Department Roles & Responsibilities Include:
- Serve as the lead response agency for public health emergencies and coordinate health emergency support in broader emergencies (e.g., wildfires)
- Provide accurate, up-to-date informationto the extent it is known
- Provide guidance and assist local health departments, if applicable
- Coordinate with CDCand other federal agencies in support of the state’s response efforts
- Lead public health emergency preparedness efforts including development of plans and response capacity
- Ensure key data and guidance is being presented and effectively communicated to the public
Key Emergency Management Office Roles & Responsibilities Include:
- Manage emergency logistics in support of the lead agency (emergency management may also be the lead agency in certain types of emergencies, such as hurricanes)
- Run point on engaging/interfacing with FEMA, if needed
- Facilitate and support resource requests from state agencies and other states
- Coordinate and support mutual aid requests for local governments
- Support agencies and government functions through continuity of operations planning and exercises, as needed
Evaluate and Enhance Current State of Readiness and Response
Readiness efforts are further enhanced by ongoing assessment of the current plans to ensure that they meet expectations, are in alignment with other applicable emergency response plans, and effectively address known and emerging threats. This process includes:
- Ensuring that the plans are actionable with the available resources,
- Identifying potential gaps; and,
- Clearly outlining steps needed to achieve the desired level of readiness.
While there may not be immediate resources available to implement all of the steps needed to achieve desired readiness, developing the pathway can help guide future activities. Preparedness activities can also include building out infrastructure for incident recovery and post-incident support. As one example, Missouri has established the Office of Disaster Services within the Department of Mental Health to plan and develop activities that support a coordinated mental health response for Missourians in disaster situations.
Leveraging the list of capability standards established by the CDC, several of which align with FEMA’s overall National Preparedness Goal and core capabilities, may be helpful in assessing current capacity:
- Community Resilience, including Community Preparedness and Community Recovery
- Incident Management, including Emergency Operations Coordination, Information Management, Emergency Public Information, and Information Sharing
- Countermeasures and Mitigation, including Medical Countermeasure Dispensing and Administration, Medical Material Management and Distribution, Responder Safety
and Health, and Non-Pharmaceutical Interventions - Surge Management, including Fatality Management, Mass Care, Medical Surge,
and Volunteer Management - Biosurveillance, including Public Health Laboratory Testing, Public Health Surveillance
and Epidemiological Investigation
In addition, the CDC’s Public Health Emergency Preparedness Program (PHEP) may provide another resource in this assessment. This program assists state and local public health departments with enhancing their public health response capabilities.
Key resources, preparedness, skills and training, and equipment and technology are also important evaluation factors. The ability to achieve the standards relies heavily on partnerships, so assessments can help clarify which entities are responsible for each standard and resources.
Practice the Plan
Practicing, or exercising, emergency plans enhances coordination and response efforts. Agencies often develop a wide array of scenarios to stress test plans, which is critical to identifying gaps and areas for improvement. Governors’ offices can also play an important role in ensuring state emergency operations plans are ready for a crisis by:
- Supporting state agency efforts to conduct interagency exercises;
- Having a representative from the Governor’s office participate in state exercises to evaluate coordination and decision-making components; and,
- Periodically practicing internal Governor’s office emergency/crisis coordination strategies to maintain readiness for an effective response.
Federal agencies sometimes coordinate or require participation in exercises to access grant funding. In addition, state agencies often coordinate and perform exercises independent of direct federal agency support.
Exercise Resources
FEMA National Exercise Program (NEP) is the nation’s cornerstone exercise program for validating progress toward promoting and sustaining a prepared nation to respond to catastrophic events. The NEP includes exercises that involve federal department and agencies, as well as State, Local, Tribal and Territorial (SLTT) jurisdictions, non-profit organizations, and the private sector. The scenarios used in these exercises often include public health emergencies, and the results are used to identify strengths and areas for improvement in national preparedness and resilience. FEMA’s National Exercise Division (NED) provides multiple resources for emergency management processionals to prepare for risks in their communities, including Exercise Starter Kits. SLTT jurisdictions may also request exercise technical assistance as part of the National Exercise Program annual Exercise Support Request process.
Governor’s Exercise Series offers a customized emergency management educational engagement for first-term Governors and their staff, tailored in duration and topics based on areas of interest. FEMA Governor Orientation (FGO), provided by FEMA Regional Administrators with support from the Center for Homeland Defense and Security (CHDS), may include a range of topics, including Stafford Act authorities; consequence management; disaster declaration processes; crisis management; federal partners, programs, and processes; and continuity of government.
Assistant Secretary for Preparedness and Response (ASPR) Technical Resources, Assistance Center, and Information Exchange (TRACIE) resource center offers a variety of resources for healthcare emergency preparedness, including exercise templates, after-action report templates, and other resources to support exercise design and evaluation.
Key Recommendations
- Review current state of readiness and adjust existing emergency operations planning to align with Governor’s priorities and maximize public safety.
- Encourage efforts to conduct emergency preparedness exercises in coordination with federal agencies and participate when possible.
- Following changes in policy, release of new guidance, or conducting exercises, assess where plans need to be improved to ensure the government is responding as effectively as possible.
Legal Preparedness
Governors’ use of executive powers through day-to-day legal authorities and under declarations during a disaster are critical to a successful response. Constitutionally, state governments have authority to make and enforce laws necessary to preserve public health, safety, and general welfare, which are vital for addressing emergencies. Additionally, state constitutions and legislative bodies have granted the executive authority power to declare an emergency and to exercise certain emergency-specific powers to better meet the needs of a state in an emergency event. These powers allow the Governor to take swift and decisive action to coordinate the state’s response and recovery efforts. However, they are also subject to legal and constitutional limitations to ensure that they are used appropriately and do not infringe on individual rights or liberties.
As much of the legal jurisprudence pertaining to Governors’ emergency authorities is developed during public health emergencies, there were fundamental shifts as a result of COVID-19. As the landscape changes, Governors and their staff work extensively to evaluate the extent of these authorities and how these powers may translate to action.
The following are key emergency legal preparedness considerations for Governors:
Identify a legal team
- Governors often establish multi-disciplinary senior response teams pre-crisis, which may include their Chief of Staff, legal counsel, health officials, emergency managers, and other experts and officials, that can be activated quickly in the event of an emergency.
- The Governor’s legal counsel is generally responsible for, or heavily involved in, preparing declarations of emergencies, subsequent executive actions, disaster relief agreements between the state and FEMA, and other memorandums of understanding between the federal government and other states.
- Proactive planning, training and relationship building between Governors legal counsel and subject matter experts may aid in a more rapid response.
Evaluate key legal tools
- Review the statutory and broader legal landscape (e.g., caselaw, administrative tools, Attorney General opinions) of the Governor’s emergency powers and/or public health emergency powers. Each state has specific laws, regulations, and procedures that dictate how emergencies are declared and managed, as well as statutory/regulatory timeframe periods and renewal limitations.
- Monitor legislative requirements necessary during an emergency (e.g., notice requirements)
and legislative changes made to emergency statutes during, and in the aftermath of, public
health emergencies. - Examine the interplay of these powers within state government and in relation to Constitutional provisions, federal law and those of local governments, particularly any gaps and overlapping authorities. Overlapping powers between state officials and between the state and localities can be complementary and provide redundancies, but careful planning and coordination is important to avoid confusion.
- Legal reviews of public health emergency authorities can also be evaluated through processes like exercises to ensure that the state is prepared when an emergency occurs. Including exercise injects on legal issues and inviting attorneys to participate in exercises can help make legal review a priority for agency preparedness activities.
- The results of these legal reviews can be integrated in plain language within plans, such as which agencies have certain authorities or the procedural steps that must be followed to take a particular action described in a plan. Doing so can provide clarity and help limit surprises when staff are carrying out a plan.
Develop a process for executive actions during emergencies
- Developing a process for drafting, vetting, and approving executive orders can help ensure swift and effective actions. This may include evaluating potential actions with a broader senior response team, external partners (e.g., Attorney General), or other stakeholders.
- Drafting template orders can save time during an emergency and create a mechanism for the aforementioned evaluation of legal tools.
Anticipate litigation
- There may be litigation to executive actions being taken. The legal team can assess the risks of taking or not taking an action, anticipate potential legal challenges, and develop strategies for defending such actions in court.
- If challenged, the order itself will be the first thing a court looks to when deciding whether to take injunctive action. Including a legal basis and justification for actions, effective dates, and other data within the order itself may provide the greatest safeguard for immediate legal challenges.
Communicate and coordinate efforts
- The Governor’s legal counsel will consult with agency legal experts, but it is important to centralize legal work so advice is consistent. Governors also frequently work with their Attorney General, as they might be defending the Governor’s actions in court. However, there have been instances where the Attorney General challenged gubernatorial actions.
- Preemption challenges arose throughout the COVID-19 pandemic as federal, state, and local governments issued orders prohibiting or mandating certain mitigation actions. To help address preemption issues, it is helpful to understand respective emergency statutory frameworks and relevant caselaw as it pertains to federal and local governments—both of which raise their own distinct and complex legal questions. On local preemption, it is particularly important to understand the relationship and scope of local decision-making control. Communicating often with local partners and other stakeholders is also critical, as it helps the public better understand and comply with emergency response actions and ensures a more coordinated response effort.
While future public health emergencies and their response will vary greatly, jurisprudence pertaining to executive authority during the COVID-19 pandemic should be considered as part of legal preparedness. Hundreds of lawsuits were brought against Governors and state officials during the pandemic. Key gubernatorial actions that faced legal challenges included the following:
- Emergency/executive authority challenges, such as scope of general authority, separation of powers and the involvement of the legislature, authority to spend federal funds, and general preemption issues.
- Challenges to social distancing measures, such as stay-at-home orders, essential business designations, temporary physical business closures, travel restrictions, limits on public gatherings (particularly religious gatherings), and other mitigation measures.
- Challenges to mask requirements or prohibitions.
- Challenges to vaccine requirements or prohibitions.
- Other related actions, such as litigation involving correctional populations, eviction moratoriums, unemployment insurance, elections, amongst others.
Generally, most state and federal courts affirmed Governors’ emergency authorities, particularly in the first 18 months of the pandemic. However, some courts, including the U.S. Supreme Court, outlined specific limitations on such powers within the context of COVID-19, particularly in cases involving religious liberty and scope of authority, and especially as the pandemic endured and emergency declarations or restrictions continued to be in place.
Balance risks and benefits
- Every action in an emergency includes an assessment of risks and benefits, which are carefully
considered by the Governor and state officials. This may include legal risks of taking action or doing nothing, broader health considerations, economic implications, and the protection of civil liberties. If the legal basis is unclear, government officials need to consider these risks and their plan to justify taking or not taking action. - When responding to emergency events, governments must balance emergency actions with civil liberties. Decisions need to be made in a way that protects constitutional rights but also provides for the health, safety, and welfare of the public in general.
- Governors use these frameworks in order to navigate their legal authority and the constitutional requirements related to both everyday emergency events as well as catastrophic emergencies.
Key Recommendations
- Identify gubernatorial emergency authorities and work with chief legal counsel to prepare to leverage those authorities during emergency events.
- Maintain a process for vetting and issuing executive orders, providing the legal basis and justification for actions within the order.
- Assess risk and balance emergency actions with civil liberties.
Funding And Resources: Administratively Preparing For An Emergency
Prior to a crisis or emergency, there are several administrative aspects of a response Governors’ offices play a role in preparing for, including identifying emergency funding streams, procurement and resource stocking strategies. Including these considerations on the front end of the planning process provides for more ready access to resources during a response. It is also important to ensure there are processes in place during steady-state so key tools are ready to be executed when necessary during
an emergency.
Funding Considerations
Funding is fundamental to responding to a public health emergency. As Governors develop their budget, they often meet with budget officials, legislators, emergency management and public health officials, among others, to better ensure emergency and rainy-day funds are sufficiently funded. It is useful to continue to evaluate the mechanisms and processes used to fund emergencies, particularly in light of growing demands on disaster response funds.
In large events in which a federal emergency is declared, the federal government may be able to reimburse expenses that qualify for the emergency response. It is important to identify which expenses qualify for reimbursement, as well as the timeline of those reimbursements to ensure that the state has a steady cash flow to respond to the ongoing emergency, in addition to maintaining other government functions. Exercising strong accounting practices, such as careful tracking of expenditures and receipts, is critical for post-incident scrutiny and auditing.
Leveraging Potential Federal Funding Sources
Before an emergency, identify the process to accept, appropriate, and expend federal funds for both preparedness and emergency response in the state. That process may vary depending on whether the authority lies with the Governor or state legislature.
Examples of federal programs for public health emergency preparedness include:
- CDC Public Health Emergency Preparedness Cooperative Agreement
- DHS Homeland Security Grant Program
- FEMA Emergency Management Performance Grant Program
Examples federal programs for public health emergency response include:
- CDC Infectious Diseased Rapid Response Reserve Fund
- CDC Public Health Crisis Response Cooperative Agreement
- CDC Foundation Emergency Response Fund
- Substance Abuse and Mental Health Services Administration (SAMHSA) Crisis Counseling Assistance and Training Program
- If declared a Major Disaster under the Stafford Act, may be eligible for Public Assistance
- Congress may also allocate funding for specified uses (e.g., the Coronavirus Aid, Relief, and Economic Security Act or “CARES Act”, and the American Rescue Plan Act or “ARPA”)
Resources and Procurement
Public health emergencies often require an increase in supplies, personnel or other resources. States will typically seek to leverage or shift existing resources first. Once the need exceeds the available resources, states may use other mechanisms, including requesting support from other states or the federal government, leveraging existing contracts or stockpiles and emergency procurement. To prepare for future emergencies, states can review and take steps to improve emergency procurement processes.
In addition to identifying the resources and capabilities on hand, it may be useful to evaluate processes on a regular basis, including who has the authority to make large scale emergency procurements, how they are funded, and what restrictions or limitations are in place (e.g. time frame, dollar amount). Many states have taken great strides to digitize and streamline their procurement processes. Below are some additional considerations as states continue to look ahead.
- Resource Surge & Contracts: Some states establish standing contracts or develop pre-approved contract language that can be used and adapted for emergencies. In many cases, vendors have similar contracts with other jurisdictions, so having an upfront understanding of what they can realistically deliver to states in those situations will be important.
- Stockpiles: Some states may elect to have state or regional stockpiles. Strategies for ongoing stockpile management have been a challenge as threats change over time and resources may have limited shelf lives. Key considerations include the types of resources stockpiled, options for rotating out stock at end of life, and sustainment funding. States are also developing different models for how they organize and distribute their stockpiles, including in some cases, contracting with a private entity who manages the stockpile and replaces items nearing expiration, among others. The HHS Administration for Strategic Preparedness and Response (ASPR) maintains a Strategic National Stockpile (SNS). The mission of the SNS is to rapidly deliver needed supplies once an emergency is declared. As states determine their own resources or stockpile needs, it is important to note that the SNS may not cover public health emergencies, larger emergencies may exceed immediate availability, and that it may take time to deliver existing inventory to the states during an emergency. For instance, HHS typically only has the raw materials for a vaccine on hand, so it may take time to get out to states. The Mpox vaccine was one of fastest rollouts and resulted in vaccines beginning to reach states in approximately a month.
Key Recommendations
- Regularly evaluate state emergency response funding levels and determine if additional funds may need to be appropriated to reserve funds, particularly given the recent rise of concurrent emergencies.
- Assess and refine emergency procurement strategies regularly along with the state’s approach to maintaining ready access to resources, including stockpiles, if applicable.
- Evaluate emergency procurement processes and legal timelines and determine if any adjustments are needed for future sustained public health emergencies.
Public Health Infrastructure & Workforce
The state’s public health infrastructure is the foundation for enactment of public health policies, maintaining healthy communities and providing needed medical care. When evaluating the systems and workforce that make up this infrastructure, it is important to factor in the capacity and resources needed to make and enact strong policy decisions during public health emergencies. This also includes incorporating avenues to quickly support and expand the responding workforce.
In some instances, states may want to consider additional investments or policies to ensure that all areas and communities in their state have equal access to services. Expanding preventive health care services and accessibility, including through programs such as telehealth, can improve immediate health outcomes as well as strengthen the resiliency of communities during public health emergencies. Other considerations may include evaluating rural public health needs and accessibility separately from larger urban areas, supporting smaller units of government in efforts to increase robustness, and expanding outreach and accessibility to underserved communities. For instance, Indiana Governor Eric Holcomb has established Health First Indiana to bolster public health infrastructure through state and local partnerships so counties can determine the health needs of their community and implement evidence-based programs focused on prevention.
Data & Data Systems: Planning for the flow of information and Governors’ offices expectations during an emergency can increase readiness. This may include discussion on public health’s syndromic surveillance capabilities, the ability of the state to collect information from localities during emergencies, as well as how that information is flowing to the Governor. Regular monitoring is important to quickly identify and respond to incidents and emergencies. Considerations for these efforts may include:
- Capacity of local health departments to capture and share health information effectively
- Infrastructure in place for data and resource needs (e.g., types of diseases, number of those impacted, number of hospital beds) to be shared quickly and securely with the state from both public and private sources
- Epidemiological and lab capacity of the state
- Availability of projections on the community impacts of diseases
- How this information is being shared to the Governor or Governor’s office on both a routine basis and when there is an incident or emergency
It may also be helpful to evaluate the current data systems in the state to determine whether they are effectively interoperable and sufficiently integrated within departments to capture and share needed information. When evaluating systems and data sharing networks holistically, it is also important to incorporate privacy and cybersecurity considerations.
Workforce: It may also be necessary to surge staffing in impacted areas, including leveraging in-state public health and healthcare workers or requesting mutual aid from other states through the emergency management assistance compact (EMAC). A Workforce Analysis can be a starting point to evaluate current staffing levels both inside and outside of government and identify where the greatest needs are. One concern during the COVID-19 pandemic, particularly for smaller states, was the need to take public health workers away from the response to perform administrative tasks in their Health Department, since they were lacking administrative staff to focus on just that aspect.
Governors’ Offices are working to build resiliency for future emergencies through workforce retention, recruitment, and flexibility initiatives. This includes providing financial incentives, reducing degree requirements for certain jobs, or incorporating teleworking flexibility. As an example, Hawai’i Governor Josh Green developed a two-year $30 million student debt repayment program in 2023 to attract more than 300 health professionals annually. This was in response to needs identified during the COVID-19 pandemic, which resulted in Hawai’i spending over $100 million for traveling nurses. This program addresses the identified need for additional health practitioners in addition to reducing long term costs.
Below are several approaches and tools that can be used in preparation for a future public health emergency:
Evaluate tasks and needed skillsets.
- Encourage response agencies to think broadly about the tasks and support functions needed to respond to an emergency, how this aligns with existing position descriptions and training, as well as how specific functions and tasks can be reassigned during an emergency. This can include mission critical functions that do not require public health expertise (e.g., data entry) and non-mission critical functions (e.g., administrative tasks).
- Support efforts to regularly evaluate and implement cross-training programs, which can be vital during a crisis when specialized skills are in high demand.
- Normalize emergency preparedness through regular training and exercise, so state employees, including Governor’s staff, understand their roles during a crisis, even if they may be infrequently needed to support a response.
Establish and leverage staffing contracts and volunteer resources.
- Work with public health officials to identify staffing gaps and frequent staffing needs during past emergencies.
- Encourage response agencies to proactively facilitate the establishment of contracts or programs that can be leveraged for additional staffing resources, ensuring that mechanisms are in place to quickly onboard medical personnel, support staff, and specialists when required during an emergency. Be mindful of whether these contracts rely on existing staff to fill the requests (e.g. a nursing contract that pulls from local hospitals).
- Support use of volunteers, such as the Medical Reserve Corps — a local network of volunteers who range from trained medical and public health professionals to other non-medical community members — as a force multiplier as appropriate.
Leverage mutual aid.
- Foster collaboration among jurisdictions, facilitating agreements to share healthcare/emergency personnel and resources when needed during public health emergencies.
- If an emergency exceeds the state or territory’s capacity to respond, resources from other states and territories can also be requested through the EMAC process. It is important to note that the requesting state or territory is responsible for paying for the resource regardless of the amount of federal disaster funding provided.
Strategize with the state’s adjutant general on use of state’s National Guard in public health emergencies.
- Enhance the National Guard’s workforce readiness by incorporating training and exercises specific to medical response, logistics, and emergency coordination.
- Ensure Guard members are well-versed in public health protocols prior to an emergency so they are equipped to provide different types of support when needed.
- Work with National Guard leadership to understand capabilities and limitations, and to be prepared for emergencies in which the National Guard may be unavailable.
National Guard Duty Status
The command and financial implications of deploying the National Guard under State Active Duty, Title 32, and Title 10 are different and provide different paths as to how they may be utilized during an emergency response:
- Under State Active Duty, the Governor is in command control of the National Guard and the state is responsible for all costs.
- Under Title 32, the Governor is in command and control of the National Guard but funded with federal dollars—which needs to be approved by Department of Defense Secretary.
- Under Title 10, the President is in command and control of the National Guard and the federal government is responsible for all associated costs.
Key Recommendations
- Analyze existing health data infrastructure, including information flow, and determine if any steps are needed to bolster systems and processes for effective use during an emergency.
- Evaluate state syndromic surveillance and other biosurveillance capabilities, and ensure they meet state’s needs.
- Explore public health and healthcare workforce resiliency strategies through all available means, including in collaboration with post-secondary education institutions and the private sector.
Public Communications & Strategic Engagement
Communication, both internal to state government and with the public, is a critical element of emergency response. As such, Governors’ offices and public health officials work to strengthen pre-disaster infrastructure to maintain situational awareness and build lines of communication with key stakeholders, both public and private, so they are fully aware of evolving issues in the community and can act more quickly.
Stakeholder Engagement
Identifying and building early relationships with federal agencies, NGOs, community organizations, and businesses, is crucial to ensuring timely coordination and preparing for a crisis. An important aspect of this is outreach to traditionally underserved communities, including working with trusted voices and community champions to distribute information. For instance, in Alaska, robust partnership and transparency between state and tribal leaders was prioritized at every point of the COVID-19 vaccination effort—emphasizing health equity and acknowledging collective historical trauma associated with previous public health emergencies.
Governors’ offices also often have direct contact with key leaders and corporations. State agencies also have existing relationships with many stakeholders that may already be organized within the state’s Emergency Operations Plan (EOP) and Incident Command System (ICS).
Stakeholders may include:
- Hospitals/Clinics
- Insurance Providers
- Public/private partners (community foundations, business / corporate stakeholders, etc.)
- Academia (local colleges, universities, HBCUs, or community colleges)
- Professional Associations (health, labor, etc.)
- Volunteer/Community organizations (Voluntary Organizations Active in Disaster or “VOAD”, Red Cross, etc.)
- Key State/Local Elected Officials
- Key Private Businesses supporting Community Lifelines (Groceries, Pharmacies, Utilities, etc.)
During a crisis, Governors’ offices help ensure all impacted stakeholders are included in the state’s emergency response. Use of ICS as outlined in the state EOP provides the framework for communication during a crisis, pre-crisis relationship building, and perspective sharing. It also helps facilitate quicker coordination and access to resources. Consistent use of these plans and structures will help ensure resources are provided in a timely fashion and limit duplication of efforts.
Communicating with the Public About Public Health
It is important to be proactive in engaging with the community at-large on health-related issues during an emergency, as regular engagement can build and maintain trust and resiliency. This engagement will be most effective when it meets people where they are, speaks to communities in ways that acknowledge their culture and perspectives, and avoids stigmatization. In addition, utilizing consistent platforms and communication methods will help the community understand where they can receive trusted public health messages in the event of a public health emergency.
This can also help to reduce the impact of misinformation and disinformation that might arise during a disaster. Tactics to combat misinformation and disinformation are discussed in greater detail in the Responding to a Crisis Section, but use of trusted voices in regular and intentional messaging through consistent communication mediums is key.
Key Recommendations
- Identify key stakeholders with whom the Governor may need to directly communicate during an emergency situation.
- Regularly engage with the public pre-crisis through consistent platforms to identify where trusted health information can be shared during an emergency.
- Develop communication strategies that incorporate messaging mediums to meet the public where they are, use content that is relatable, digestible, and speaks to the culture and community you are trying to reach.
RESPONDING TO A PUBLIC HEALTH CRISIS
This section is intended to be an action-oriented guide to enact state plans and preparedness efforts in an effective response. For additional details and background on the actions presented, please refer back to the preparedness section of this guide.
Governors prioritize making well-informed decisions during emergencies based on the available information, recognizing that the evolving nature of emergencies often requires quick and thoughtful judgment. This is why when a crisis arises, it is important that critical information is quickly and effectively communicated, and that plans and processes developed and exercised in preparedness for an emergency are quickly and effectively deployed.
The nature of the emergency will influence how a Governor may respond. The section below provides potential steps Governors’ offices may want to consider as well as additional context on how a response may be executed.
Evaluate Incident & Level of Response Needed
When a potential public health emergency is reported, the response may vary based on a number of factors, including the risk to the public, potential for spread, prophylaxis and treatment options, as well as the capacity of the jurisdiction to respond. For public health threats reported in nearby states, Governors’ offices may also choose to work with public health officials to monitor for future potential impacts and ready resources to respond. Below are some potential steps Governors offices can take to evaluate and monitor an incident:
Assess the situation and identify immediate necessary actions.
- Work with public health officials to identify the scale and severity of the public health threat; this may include factors such as number of individuals impacted, rates of morbidity and mortality, and potential for spread.
- Contact local authorities in impacted communities to open lines of information-sharing and to offer support and resources.
- Identify any potential safety measures that the public can take and determine how best to share that information.
Evaluate information needs.
- Identify whether additional data collection is needed to make informed decisions.
- For incidents or illnesses that are novel or have an unknown cause, work with public health officials to determine a timeline to identify the source and potential for spread or additional incidents.
Monitor initial impact and assess next steps.
- Evaluate and monitor available resources and capacity to respond, as well as whether additional resources may be needed.
- Coordinate with HHS and FEMA, as appropriate.
- Monitor the situation and continue to evaluate what additional action may be needed.
Activate Incident Response Plan
When a public health emergency is identified, Governors’ offices may consider activating the relevant components of their incident response plans. As outlined in the critical incident planning section of this document, the Incident Command System and the Emergency Operations Plan can provide a framework for a response that can be scaled to the scope and severity of the incident. Depending upon the assessment of the situation, it may be important for Governors’ offices, public health, and emergency management officials to meet on a regular basis to allow for responsive decision-making and information flow.
Key actions during the activation may include:
Initiate increased reporting and regular touch points with key leadership.
- Identify the meeting tempo for key staff or policy group meetings. This tempo may vary based on the scope, scale, and pace of the emergency (twice daily, daily, weekly, or ad hoc).
- Identify the reporting tempo for situational updates from key responding agencies either more regularly or in sync with the identified meeting tempo. If there are expectations on specific information requirements and format, a template can assist in streamlining information flow.
- Coordinate with key private sector partners (e.g. hospitals, insurance companies, etc.) to gain a stronger situational awareness of the response needs and potential threat impacts, including resource availability/demand, capacity of healthcare facilities, and any emerging challenges.
Identify needs of primary responding agency.
- Communicate with the primary responding agency and ask what their immediate needs may be, including personnel, equipment, supplies, information, and funding. The primary responding agency is typically the one with the most direct responsibility for managing the response. For example, in a situation involving the spread of an infectious disease, the primary responding agency might be the state’s Department of Health.
- Identify the primary responding agency’s current capabilities and resources, and any available thresholds or triggers for requests of additional support.
- Monitor evolving needs and adjust the response accordingly.
Declaring an Emergency & Subsequent Executive Actions
Gubernatorial emergency powers are generally activated through the implementation of a state declaration or proclamation of emergency or disaster. Although statutory schemes vary, all states give the Governor authority to declare one or more types of emergencies, including a disaster emergency or a public health emergency. State laws specify how these legal declarations are made, durational limitations, legislative involvement, and other potential constraints. While unique to each state, an emergency declaration generally addresses the effective dates and duration of the declaration, geographic areas covered in the state, conditions giving rise to the emergency, applicable response actions, and the agency leading the response activities.
The following are key steps when declaring an emergency and issuing subsequent executive actions:
Prepare for the declaration.
- If the situation goes beyond the management capability of local or state entities, Governors and their senior teams will determine which type of emergency, if any, is most appropriate for the situation and who is the most appropriate individual to make it (e.g., Governor or state health official).
- Once the determination is made, the Governor may then direct the legal team to prepare necessary documentation, outlining the reasons and legal basis for the declaration. Carefully outlining justifications for actions and their relation to the emergency may help executive orders better withstand potential legal challenges.
Draft and define objectives of the declaration.
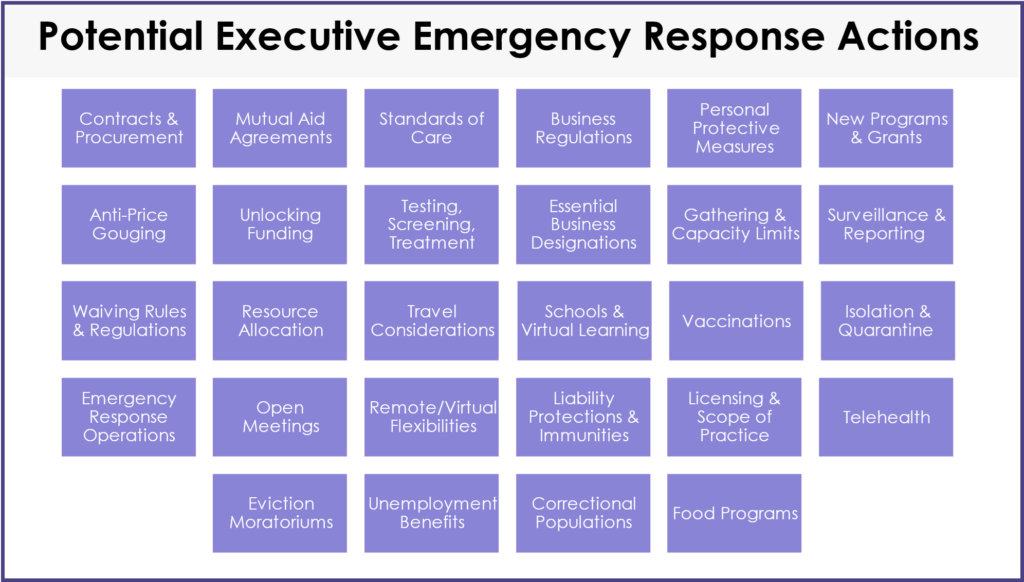
- Direct staff to draft a declaration that addresses issues identified in the state investigative process and clearly define the objectives, scope of impact, any applicable enforcement mechanisms, and expected duration of the order. See Figure 3 for more information on potential objectives.
- When drafting, Governors’ offices may need to balance the need to craft discrete outcomes or metrics to manage the public’s expectations on when the declaration may end against allowing for sufficient flexibility to meet the evolving challenges and community needs.
Declare the emergency and/or take other executive actions.
- Communicate the declaration to the public, providing clear and concise information about what the declaration means and the actions being taken, as well as any other information on steps the public should take to protect themselves.
- The Governor may also discuss any data metrics, what success can look like, next steps and what the public should expect, and how the emergency phase will end.
- Keep the public informed and provide regular updates on the emergency declaration to promote compliance and increase awareness of any public safety or public health concerns.
- Depending on the type of emergency, Governors may also request a federal declaration.
- For a federal emergency or disaster declaration request pursuant to the Stafford Act, the Governor must submit a request to the President through the appropriate FEMA Regional Administrator within 30 days of the occurrence of the incident. If the total amount of federal emergency assistance provided exceeds $5 million, the President must report that information to Congress.
- For a Federal Public Health Emergency, a Governor is not required to formally request the HHS Secretary to make a declaration, but the Governor can also work with the HHS Regional Emergency Coordinator at their regional HHS office who can help facilitate the request.
- Implement or request waivers needed to aid in response or expand access to services in impacted communities. This may include the suspension of specific safety regulations, such as Federal Motor Carrier Safety Administration (FMCSA) hours of service restrictions for motor carriers and drivers engaged in certain types of emergency response, or Social Security Act 1135 waivers for certain Medicare, Medicaid, Children’s Health Insurance Program (CHIP), or Health Insurance Portability and Accountability Act (HIPAA) requirements to help beneficiaries access care.
Evaluate and amend orders and actions as needed.
- Once the declaration is implemented, the Governor and senior response team continuously monitor the impact, making adjustments as needed, to ensure effectiveness. This may come in the form of subsequent executive orders, directives, or state agency actions.
- Establish a clear pathway for agencies and other stakeholders to report challenges impeding the response that may require additional executive orders or amendments to current actions to address them.
- If the declaration requires renewal after a prescribed period (e.g., 30 days), continue to outline and update the justification and response efforts included within the order.
- Prepare to update and amend executive actions in response to litigation and legal challenges if specific limitations are outlined by a court.
EXTENDING A DECLARATION
Determining when to renew or rescind an emergency declaration is a multi-faceted decision, especially when responding to a novel disease or evolving disaster. Preserving statutory and regulatory flexibility during emergencies allows Governors and state officials to quickly implement response efforts that will save lives. Depending on the extent of the emergency and impact to the community, Governors may have to weigh different considerations related to implementing public health mitigation efforts and various economic and social realities that impact the continuity of daily life. Ultimately, Governors may opt to keep declarations in place to ensure the state has the ability to adjust and recalibrate response efforts with the ever-changing landscape of the emergency.
Planning for sustainability and transitioning to recovery.
- Ensure response operations are prepared to transition to normal authorities in advance of an emergency declaration or executive order lapsing.
- Evaluate if permanent legal or regulatory frameworks need to be amended or adjusted because of authorities or actions that may be needed in the long term.
Obtain and Allocate Resources
In times of crisis, resource planning is essential for effective emergency response. Governors and their teams engage in ongoing comprehensive resource evaluation and collaborate with public and private sector partners to ensure the success of a sustained response. This section outlines key considerations in resource assessment and proactive procurement to enhance the response in addressing public health emergencies:
Evaluate resource needs.
- Obtain regular updates from public health officials on data obtained through their collaboration with healthcare providers, laboratories, and other relevant entities to systematically evaluate real-time data on things such as hospital bed availability, personnel, PPE, ventilator usage, etc.
- Evaluate whether current data collection is adequate to answer policy considerations. If not, seek ways to increase reporting, as allowed by law. Consider looking at ways to provide support if this increased reporting would be overly burdensome and may impact response.
- Consider developing a data dashboard to establish a central location for needed information and enable better information sharing across sectors and the public.
- Work with subject matter experts to leverage existing data, such as the likely number of individuals impacted, resource availability, and the burn rate of needed resources, to forecast future requirements.
Initiate processes to obtain needed resources.
- Develop an adaptive procurement team and structure for evolving conditions.
- If the state has stockpile(s), work with responders to determine how those resources might be best leveraged based on the type of emergency and resource availability.
- For limited resources, prioritize allocation of available resources in the interests of public safety (e.g. responders, vulnerable populations) while additional resources are procured.
- Direct staff to identify existing contracts to tap into or procure additional supplies if needs are below required procurement thresholds.
- Determine if emergency procurements are needed to fill additional resource needs that cannot be covered with existing capacities. Where available, utilize existing contracts and stock contract language for quicker execution.
- Continue to direct staff to track resources expended for auditing purposes, and in case they are or become eligible for federal reimbursement.
- If appropriate, consider submitting a request to the Strategic National Stockpile (SNS). To request assistance from the SNS, the Governor or senior health official will need to submit a request to the HHS Secretary or HHS Secretary’s Operations Center.
Engage with public and private sector partners.
- Work with key private stakeholders, including those identified while preparing for a crisis, in impacted areas to determine what, if any, resources or services are needed to support continued operation of essential services (e.g. utilities, pharmacies, grocery stores).
- Work with private sector partners, including businesses or the non-profit community, to determine if they can offer assets to assist in the response.
- For businesses, this could include expanding manufacturing capabilities for PPE, providing warehouse space for supplies, assisting with data infrastructure, or identifying local parking lots to establish a vaccination site or community resource distribution center, among others.
- For the non-profit community, this could include receiving/distributing donations (physical or cash) and/or volunteer management.
Work with the state’s adjutant general to assess the potential need for National Guard resources.
- Direct staff to determine the specific tasks that are not currently being performed due to limited existing capabilities that the National Guard can support. This may include tasks such as distributing supplies, filling critical staffing roles, or managing testing/vaccination sites.
- Determine the urgency of the task and if the National Guard is able to mobilize quickly enough to fill the need or if another resource may be better suited for the situation.
- Consider deployment options, whether they will be on state active duty, or if a request needs to be made to the President or Department of Defense Secretary for a Title 32 activation.
Work with public health officials to consider activation of the Medical Reserve Corps or other volunteer organizations.
- Direct staff to determine if there are tasks best suited for the Medical Reserve Corps or other volunteer organizations.
- Engage with the Medical Reserve Corps or other volunteer organizations, understanding these are free resources, and monitor morale.
Leverage data to justify requests for additional resources from other states, federal partners, or the state legislature, if needed.
- Direct staff to determine if there is a need to request assistance from other states through the Emergency Management Assistance Compact (EMAC). Be sure staff identify how EMAC requests will be paid for and whether costs will be reimbursed by the federal government. Make strategic requests based on the amount of time it may take for responders to arrive in response to the state’s request.
- Charge response agencies with determining whether any standing or emergency federal resources and/or teams may be able to support the response. For public health this may include leveraging the agency for Toxic Substance and Disease Registry within CDC for emergencies involving hazardous substances or the CDC Global Rapid Response Team, etc.
Work with the state legislature, particularly during an extended emergency, to pass appropriate legislation to support response and mitigation efforts, including additional authorities and appropriations, as needed.
Budget Management
Governors continually evaluate budget demands and monitor resource constraints throughout emergencies. By proactively directing staff to address budget considerations and explore additional financial strategies, Governors prepare their states to more effectively respond to and recover from public health emergencies. Below are potential steps Governors’ offices can take during a public health emergency to ensure effective budget management:
Engage in ongoing discussions with response agencies to assess the status of the state’s disaster funding.
- Continuously evaluate the capacity of agencies to reallocate resources to meet current needs. Agencies may have varying abilities to redirect funds, and fiscal year-end considerations may impact available funding. Collaboratively strategize on resource allocation to optimize the state’s response to the crisis.
- Direct agencies to track and continually evaluate costs associated with staffing (including the increased number of personnel, hours/overtime, and any staffing contracts), procurement of supplies and equipment, response infrastructure needs (such as the setup of temporary healthcare facilities or the retrofitting of existing spaces to accommodate healthcare needs), and the increased demand for public services.
- When deploying resources such as the National Guard or EMAC, factor these expenses into budget planning to ensure sustained cash flow for the broader response effort.
Identify and leverage potential federal funding sources.
- Collaborate with public health agencies to identify and request specific funding sources designed to address public health crises. Explore available federal health grants and assistance programs, such as the CDC Public Health Crisis Response cooperative agreement, among others.
- If a Stafford Act declaration is issued, ensure emergency management officials determine allowable costs for federal reimbursement and non-federal cost-sharing requirements. Align budget planning with any reimbursement guidelines.
- Depending on the scale and duration of the emergency, Governors may also seek to work with their Congressional delegation to request a federal appropriation, including annual, supplemental, or continuing, passed by Congress and signed by the President, for additional financial support.
- For longer-term emergencies, such as the opioid crisis or endemic diseases, Governors’ offices can work with agencies to identify available federal grants.
Evaluate the need for changes to state appropriations.
- Work with the legislature to secure additional funding and budget authorities, as needed.
- Factor recovery needs and programs into future budget development.
- For longer-term emergencies, direct agencies to include new programs or identify resources and funding needed to adequately address the crisis in their budget proposals.
Monitor spending and ensure effective record keeping.
- Establish rigorous record-keeping practices within state agencies responsible for disaster response. Accurate and detailed records of disaster-related spending are essential for auditing and reimbursement requests.
- Ensure that these records adhere to federal and state financial regulations.
Communicating during a Public Health Emergency
Governors, along with state and local public health officials, are a key voice during a public health emergency. Proactive communication that provides actionable updates for local communities and responsive communication that acknowledges and addresses community concerns are essential components of any successful communications approach during a public health emergency. Below are considerations to assist in aligning messaging, reassuring and educating the public, and conducting effective media outreach, with a particular emphasis on engaging hard-to-reach communities and responding to misinformation and disinformation.
Align on Messaging.
While challenging during times of crisis, message alignment is a crucial component of an effective response. Governors’ offices play a key role in ensuring agencies are amplifying key messages through a coordinated flow of information, as well as ensuring that responses to messages from the community are being monitored to understand if there may be any confusion or misinformation spreading.
- Direct staff to ensure there is a clear process for controlling the flow of media requests and public communications.
- If a Joint Information Center, a component of Incident Command System (ICS), is stood up, ensure it is factored into the information flow process as it can assist in getting a Governor’s message out to agencies, while also providing an opportunity for agencies to request guidance on the questions they are receiving.
- Direct staff to develop a process for verifying incoming information with subject matter experts and to identify what is unknown or potential misperceptions to ensure accuracy prior to making a decision on whether to share publicly.
- Make messaging (statements, press releases, talking points, press conference Q&A, etc.) available on multiple public platforms to allow for the greatest public access.
- Ensure appropriate qualifiers are added to public messaging so that the community has a true sense of the information being shared. Speed and accuracy are hard to balance, but sharing information quickly while managing the public’s expectations can help minimize the spread of rumors.
Communicate regularly with the public.
- For no-notice events (e.g. the spread of a novel infectious disease or an industrial incident), determine if an immediate statement from the Governor should be released once a public health threat is identified to make the public aware and shorten the duration of any information vacuum.
- While limited information may be available at this stage, alerting the public to the threat and assuring them that their government is taking steps to learn more, may help assuage initial public concerns.
- For advance-notice events (e.g. a hurricane), provide proactive communications on steps individuals can take to protect themselves from any resulting public health threats.
- For events that may disrupt public access to traditional communications methods (TV, social media, etc.), determine alternative communications methods (wireless emergency alerts through the integrated public alert and warning system [IPAWS], emergency alert system, radio, etc.).
- Ensure messaging across the government is clear, timely, focuses on the safety of the public and provides realistic timelines for the response and the recovery from the emergency.
- Regularly collect and amplify the actions the state is taking directly, or in conjunction with stakeholders, to protect the public so individuals are aware of the government’s actions and where they can access needed resources.
- Provide regular updates on the public health threat so individuals can make informed decisions on the best ways to protect themselves and their families.
Conduct media outreach.
Print, audiovisual, and social media campaigns present opportunities to share accurate and timely information about the crisis as well as recommended actions for the public to take — playing an important role in mitigating the impact of a public health threat. Below are considerations for Governors and their offices as they work to engage with their communities through a variety of mediums:
- Engage regularly and consistently with the media (keeping in mind that the frequency may depend on the nature of the public health threat).
- Establish a consistent engagement timeline with the media (this will help reduce the volume of ad-hoc questions received from multiple media outlets).
- Direct staff to develop and issue proactive communications that advance the Governor’s messaging and guidance.
- Proactive communications may be prioritized over ad-hoc media requests, as the information can reach larger audiences; however, staff should work to maintain media relationships and answer ad-hoc requests when able.
- Consider holding a press conference or sharing a press release for information that needs to be conveyed to the largest audience possible (1-on-1 interviews may be better suited to deliver tailored messaging to a certain audience or for the Governor to provide more context on the decision-making process).
- Preparing for and addressing difficult questions head on is important for successful engagement through these mediums.
- Leverage social media platforms such as Facebook, Instagram, X (formerly known as Twitter), among others as additional avenues to amplify messaging during an emergency.
- While creating unique content for each platform is generally good practice during steady state, it is advisable to cross-post the same content to each platform to save bandwidth for creating more content and maintaining consistent messaging that keeps the public updated and informed.
Develop informational hubs.
Recent technological advances have made it easier for Governors to swiftly and accurately share data that can help constituents understand the current state of public health emergencies. Below are a few considerations in developing central information resources that can be distributed through a hub-and-spoke model:
- Develop incident-specific websites that contain access to resources, frequently asked questions (FAQs), updates on state government actions, and updates on the public health threat overall.
- Incident-specific websites (“hubs”) can provide a central space to which to redirect communities through a variety of different mediums and channels (“spokes”), and their use reduces the number of areas where outdated information may exist on public websites.
- FAQ pages also provide useful information to constituents that reduces the amount of incoming communication and creates more bandwidth in other areas.
- Employ data visualization tools to effectively communicate key trends (geographic, demographic, etc.) that help amplify key messages.
- Effective data visualization tools distill complex data into an approachable, accessible format that is easily digested by constituents.
- Adapt communication methods to suit the preferences and needs of different constituencies or private partners as needed. This may involve specific email updates, webinars, conference calls, or customized briefings that cater to the specific interests and responsibilities of each partner.
- Consider establishing a dedicated web portal or email distribution list to share relevant updates with private sector partners.
- Provide tailored information on industry-specific guidelines, business continuity plans, and resources available to support their operations during the crisis.
Engage communities who may be underserved or vulnerable.
Comprehensive and holistic community-driven communication tactics are essential to building a successful emergency response. Certain constituencies may require additional and specific communications, and below are a few key considerations for Governors and their offices to reach them:
- Identify key constituencies that may be either at a greater risk from the public health threat, such as those who rely on medical devices, older adults, infants, individuals who are pregnant, or individuals who may be underserved and needing additional attention.
- Identify the best avenues to reach individuals in these constituencies with key health information.
- Collaborate with trusted community leaders and champions to support the state’s public health emergency communications efforts:
- Obtain input on the best way to share information, including the delivery medium and the language used. For instance, print media, printed materials in local businesses or billboard advertising may have a greater reach and impact in some jurisdictions versus others.
- Collaborate on distributing health information and the message itself to maximize the effectiveness of its reach, as well as work with community leaders as a conduit for questions from the community that need to be addressed.
- Ensure information shared is accessible. This may include making it available in multiple languages, as well as ensuring individuals with a disability are also able to interpret the information.
- This may include the use of interpreters at press conferences, close captioned social media videos, and ensuring websites have accessibility features.
Stay alert for misinformation & disinformation.
Adversarial nation-state actors may seek to take advantage of an emergency to share disinformation in an attempt to sow distrust with the government. Additionally, the growth of a variety of social media platforms has allowed individuals to share information more widely, more quickly, which may increase the amount of unintentional misinformation being shared. Governors and their offices must take this into account during a crisis. Below are some strategies to consider in addressing misinformation and disinformation:
- Use consistent methods and platforms to communicate intentionally and transparently during a crisis.
- Direct communications staff to monitor current narratives to identify potentially harmful misinformation or disinformation that may need to be addressed or debunked.
- Work with the local community leaders and community champions to address targeted disinformation in their communities.
- Develop a Rumor Control website or provide public access to regularly updated FAQs.
- Monitor the types of questions received from the public, either through social media, phone calls, or in-person, and adjust external messaging (through FAQs, a Rumor Control Website, press conferences, and/or direct engagement with community leaders) to address common themes.
- In all communications, direct the public to official websites and trusted sources of information.
- Use government platforms to address common or highly publicized misinformation, but do not directly engage with low-reach social media posts promoting misinformation or disinformation, as that may draw more public attention to it.
If warranted, work with federal agencies to alert the public that nation-state actors are sharing disinformation to undermine the response to the crisis.
POST-RESPONSE & RECOVERY
In the aftermath of a public health crisis, effective post-response and recovery efforts are paramount to fostering healing in communities and preparing them for the future. Depending on the nature of the public health threat, recovery can be a prolonged process, spanning years or even decades. This section outlines strategies for monitoring long-term health impacts, maintaining open communication channels, evaluating mental health and well-being, conducting evaluations of the response to improve for the future, and providing timely and tailored information to stakeholders. Below are a few areas Governors and their offices may consider as they work toward a comprehensive and resilient recovery process that acknowledges the potential for extended timelines in rebuilding and healing.
Monitor Long-Term Health Impacts & Potential Need for Additional Support
- Monitor any long-term health impacts from the public health threat, particularly for vulnerable populations, including among others maternal and infant health, as well as the potential subsequent effects on the recovery of communities across the state.
- Continue to work with health officials to monitor epidemiological surveillance and any subsequent incidents, as well as adjust resources as needed to mitigate the impacts.
- Evaluate any needs or gaps in resources that may require additional local, state, or federal assistance.
- Direct staff to assess what gubernatorial authorities may be available to mitigate post-crisis effects, as well as what role the state legislature and municipal government play in those efforts.
Evaluate Mental Health and Well-Being
- Work with public health officials to conduct a mental health needs assessment to assess risk factors and at-risk groups. This can help determine the need for additional or targeted mental health services and education.
- Monitor and provide access to mental health resources to impacted communities, and work to meet constituencies where they are in the community. For example, provide resources directly through schools for emergencies that impact children and young adults. One tool that could be utilized to expand crisis counseling capabilities includes the Substance Abuse and Mental Health Services Administration (SAMHSA) Crisis Counseling Assistance and Training Program that is funded through FEMA for Presidentially Declared Major Disasters.
- Inform the public on available mental health and well-being resources and look for ways to reduce barriers to participate. These include access to crisis counseling or call lines, such as 988 or the SAMHSA Disaster Distress Helpline, among others.
- Evaluate whether available services meet the cultural and language needs of the impacted communities and seek outside resources as needed to fill identified needs.
- Assess and determine if additional support for disaster responders’ mental health may be needed.
- For a prolonged response and recovery, review the needs of impacted communities regularly as mental health and well-being may be further affected by the extended nature of the incident.
Continue Regular Communications on Recovery
- Even once the immediate threat is over, continue to communicate with the community-at-large, including intentionally reaching out to underserved communities, regarding recovery and any long-term impacts.
- Regularly inform the community on the recovery process and how to navigate available recovery resources and assistance. This may include re-orienting existing response websites or portals to share more information on the different types of recovery assistance available.
- Continue to share relevant updates, guidance, and actions with public and private sector partners in a timely manner. This includes information related to the transition from response to recovery, available resources, and changes in guidelines or regulations.
- If federal resources are available for recovery, task agencies with providing information to support communities in navigating the assistance process.
- Release regular updates on the recovery to help outline clear expectations to the public on what actions they can continue to take, as well as what the state is continuing to do.
- Intentionally provide opportunities for community feedback to allow for better situational awareness of any gaps or lingering issues in the response.
Conduct Post-Response Evaluation
- Direct staff to complete a post-response evaluation or an After-Action Report to review the effectiveness of the response to mitigate the impacts of the public health threat, and to determine whether changes should be made for a future public health emergency. Capture lessons learned from all staff levels and memorialize institutional knowledge to ensure information is passed on for use in future emergencies.
- Ensure stakeholders, such as state agency heads, public/private partners, and other community stakeholders, are included in the assessment to provide a more holistic review of the response.
- Strengthen identified areas that were successful, while adjusting areas that need improvement so that the state is better prepared for a future public health emergency.
GLOSSARY
Emergency Management Assistance Compact (EMAC): A mutual aid agreement among states and territories that enables them to share resources during a crisis by coordinating between various agencies and local responders, as well as offer training to ensure the readiness of emergency management personnel. States requesting support from other states through EMAC are responsible for paying for the assets provided.
Incident Command System (ICS): A standardized management framework for coordinating and managing resources, personnel, and activities during emergencies to ensure effective response and decision-making. It promotes clear communication and coordination among various agencies and responders.
National Preparedness Goal: Established by FEMA, this goal outlines a broad national vision for emergency and disaster preparedness by identifying 32 core capabilities necessary to achieve that vision across five mission areas: Prevention, Protection, Mitigation, Response, and Recovery. Although only one of the 32 core capabilities within the National Preparedness Goal specifically focuses on public health and medical support (Public Health, Healthcare, and Emergency Medical Services), many of the core capabilities relate to and contain public health and medical considerations that are necessary to successfully achieve a secure and resilient nation.
One Health: A collaborative, multisectoral, and transdisciplinary approach to public health with the goal of achieving optimal health outcomes recognizing the interconnection between people, animals, plants, and their shared environment.
Preemption: A legal doctrine that allows higher levels of government to restrict or even prevent the power of a lower level of government to regulate a specific issue. Under the Supremacy Clause of the US Constitution, federal law supersedes conflicting state and local laws either expressly or implicitly. Preemption may also be applied by states to limit cities, counties, and other lower-level municipalities ability to legislate or otherwise implement rules across a broad array of issues. The extent of a state’s ability to preempt local government depends on a variety of factors, including the state’s statutory scheme and the type of activity that is being regulated.
Steady state: The normal, day-to-day operational condition of an organization or system when there is no ongoing crisis or emergency.
Strategic National Stockpile (SNS): A program managed by the U.S. Department of Health and Human Services (HHS) that stores large quantities of pharmaceuticals, vaccines, medical supplies, and equipment to provide a fast and effective response to public health emergencies, including pandemics and bioterrorism events.












