States continue to drive toward improving the health of their residents and, because health care costs are a large and growing component of state budgets, governors also are looking for long-term, transformational ways to improve the efficiency of their Medicaid programs. Generally, a small segment of the enrollee population account for large portion of states’ Medicaid expenditures. Those individuals with complex care needs, also known as “super-utilizers,” tend to have a history of chronic illness, multiple comorbidities, special needs and other non-clinical complications that may be related to unstable housing, employment, food and transportation and interaction with the criminal justice system. They often use emergency departments and inpatient services when home and community-based interventions could be employed with good outcomes and at lower costs. By appropriately redirecting state funds to address the comprehensive needs of people with complex care needs, states can rein in escalating costs and improve the quality of care delivered to high-risk and vulnerable Medicaid beneficiaries.

State Strategies to Support Marketplace Plan Enrollment as the Medicaid Continuous Coverage Requirement Winds Down

State-Driven Initiatives to Support Moving to Value-Based Care in the Era of COVID-19

BALANCING MEDICAID BUDGETS AND SERVING STATE RESIDENTS DURING A PANDEMIC

State Strategies to Advance Health Data Interoperability

A Strong National Economy Depends on Strong States and Territories

Supporting A Trained Direct Care Workforce In Facility Settings During And After The Covid-19 Pandemic
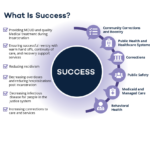
Associations Release Roadmap on Strategies for Countering Opioid Misuse in Correctional Settings

Expanding Access to Medications for Opioid Use Disorder in Corrections and Community Settings

Maternal and Child Health Update 2020