Increasing COVID-19 vaccine uptake among children is a complex challenge that will likely require many different strategies from Governors.
(Download)
Throughout 2022, the National Governors Association Center for Best Practices (NGA Center) partnered with the Behavioral Insights Team (BIT) to help Governors’ offices and state leaders develop effective COVID-19 vaccine campaigns. In a nine-month learning lab, state teams of three to four representatives convened in bi-weekly workshops to leverage BIT’s deep knowledge of applied behavioral science while developing accessible, timely campaigns. As part of the workshops, state teams wanted to learn which messaging strategies were evidence-based and most successful, but few messages had been tested specifically for COVID-19 vaccines. To fill this gap in evidence, BIT created an online trial to generate new learnings to inform states’ approaches to messaging.
During the learning lab, BIT presented potential concepts for an online experiment. State teams shared barriers they faced in administering the COVID-19 vaccine for children and most participants supported a trial focused on exploring pediatrician-caregiver interactions. With this input, BIT conducted a trial with the goal of determining the best way for pediatricians to introduce the pediatric COVID-19 vaccine to parents and caregivers. While the messages tested did not increase vaccine confidence for the participants, the trial results point to other valuable insights.
Vaccine Hesitancy Is a Complex, Long-Standing Issue
Despite its lifesaving benefits, some have been wary of COVID-19 vaccines since their introduction. However, vaccine hesitancy and misinformation have always been part of the public health landscape, dating back to the 1800s. The United States has seen considerable change and social uncertainty prior to and through the COVID-19 pandemic, fueling hesitancy and misinformation around the vaccine, especially related to vaccinating children. Many parents have decided to wait to vaccinate their child or forgo immunization against COVID-19 completely. As of February 1, the Centers for Disease Control and Prevention (CDC) reported that less than one-third of children aged 5 to 11 had been fully vaccinated, and only 1 in 10 of those 4 and under had received the vaccine (Figure 1). The CDC also reported that vaccine rates vary across states, ranging from two percent to 100 percent, depending on the age group. Other routine childhood immunizations have also been affected by vaccine hesitancy and COVID-19-related disruptions, as overall rates for state-required vaccines declined by two percent since the start of the pandemic—a significant decline for many vaccine-preventable diseases.
Figure 1
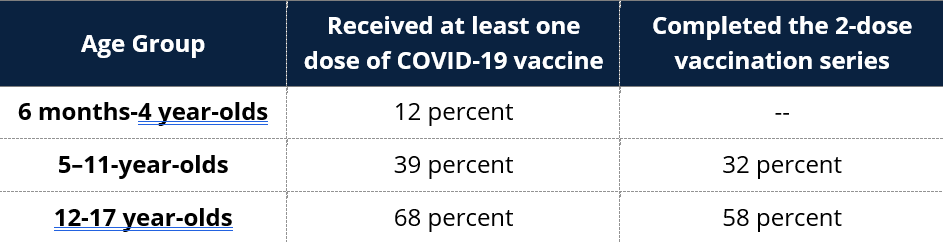
Testing Messaging Online
Using Predictiv, BIT’s online platform for conducting behavioral experiments and surveys, BIT ran a trial to better understand how states might use different types of messaging to improve vaccine confidence and uptake. With Predictiv, BIT was able to test whether specific messaging worked before implementing it in the real world.
BIT tested three behaviorally-informed messages introducing the pediatric COVID-19 vaccine to a parent or caregiver during a routine appointment. Over 6,000 parents and caregivers with a child between six months and eleven years who has not yet been vaccinated against COVID-19 participated.
First, participants saw one of the messages from a pediatrician, who are commonly seen as a trusted source of information (Figure 2). Then, the participants were presented with questions as if they were at a regular checkup. BIT measured the responses, specifically, whether parents intended to vaccinate their child during the hypothetical checkup or if they were willing to continue discussing the vaccine.
Three Evidence-Based Messages
The first message used a presumptive style which presented vaccinations as the default. This messaging normalized the vaccine, with the goal of creating a more comfortable environment for the parent to discuss their concerns. Presumptive messaging or “opt out” options are associated with higher acceptance of vaccines and screenings, including for the human papillomavirus vaccine and testing for sexually transmitted infections. The second technique used a message focused on urgency to motivate parents to act. This message was designed in line with the Protection Motivation Theory, which states that people are more inclined to act if they feel like they can avert a risk, e.g., catching COVID-19. The third message was fact-based, highlighting personal health risks associated with going unvaccinated. This approach using “personal risk frames”, has been used in other public health campaigns to promote healthy behaviors such as quitting smoking. Figure 2 shows the specific messages that were tested against a control where the vaccine was introduced with no additional context.
Figure 2

Null Results Point to Other Promising Insights
While the findings did not show a significant statistical difference between the test messages and the control for participants who were receptive to the COVID-19 vaccine, there is still much to learn from this result. It also shows how deep-rooted parents’ questions or concerns about the pediatric COVID-19 vaccine, which underscores the potential need for states to work with pediatricians to engage in more intensive, informative conversations to better answer questions or alleviate concerns.
This trial also provided evidence that the presumptive message was particularly ineffective for vaccine hesitant groups (i.e., parents who are not fully vaccinated themselves). Although this type of messaging is still useful in many contexts, based on this result, states may want to consider that starting conversations with simpler, more casual introductions may make these groups more receptive. In contrast, parents and caregivers of children under five who identified as fully vaccinated showed more overall receptiveness to the vaccine regardless of the message presented in the test.
Increasing COVID-19 vaccine uptake among children is a complex challenge that will likely require many different strategies from Governors. To increase overall confidence and uptake, more research is needed to understand hesitancies and identify strategies to mitigate them. NGA is continuing to work with states to help them address vaccine confidence for COVID-19 and beyond as they focus on increasing access, improving data sharing and combating misinformation.
Contributions by Eden Moore and Michelle LeBlanc












